Amber’s Important Message for Self Advocacy and Positivity at 25
Learning from Amber Woods: A Message of Self-Awareness, Advocacy, and Positivism
Hello everyone.
Welcome back.
By now, you’ve probably heard of Amber Woods’ story.
It’s pretty scary because you kind of wonder to yourself,
“How does a young woman with her whole life ahead of her have a disease that usually appears in people that are 60 years old and up?”
And that really calls into question our own hopes and dreams.
So, we tend to ask ourselves, “If this can happen to her, what if it happens to me?”
That is where Amber’s message of self-awareness and self advocacy gets its beauty.
Because while I might be prone to a woe-is-me mentality, it seems like she has the ability to take a negative and transmute it into a positive.
So, I’m hoping I can promote her message a little bit further by offering some of my own insights.
So that you have the tools you need to guide a conversation with your doctor more deliberately, more intentionally.
So that you can get to your diagnosis faster, get to your treatment faster, and be more present with your family and loved ones.
So, let’s get started.
Decoding the Doctor’s Process: Why Things Get Missed
The Pattern-Matching Framework
As I was mentioning before, her story is pretty incredible.
She mentions on her social media that for a while she was diagnosed with acid reflux.
And for a time it seemed to be the only thing that makes sense.
But at some point her acid reflux got so severe that she had to go to the emergency room.
And when they ran a few tests, they realized the real diagnosis.
So why didn’t anybody see this coming?
It has to do with how your doctor looks for patterns.
So, we’re going to walk through how your doctor might be thinking through things.
We’re going to talk about:
- Why something might be missed
- The early signs that we need to pay attention to
- What kinds of questions to ask your doctor when your symptoms don’t go away and you feel like there is a legitimate problem
- And how to do it in a way that there is a real partnership in figuring out what’s going on.
And so in this way, you’ll be able to tease out whether or not a symptom is hiding a more serious diagnosis because we always expect that a serious illness is loud and obvious.
We always assume that a problem is sudden, like a heart attack or a stroke, or you can’t feel one part of your body.
But that’s not always true.
Even the heart attack or stroke has the canary in the coal mine.
Certainly, it may be sudden and you’ll never see it coming, but usually there’s something to pay attention to.
There’s something to notice.
And that’s what doctors usually look for.
They’re not trying to ignore you.
They’re not trying to ignore your symptoms.
What they’re trying to do is figure out what is the most likely cause of what you’re experiencing right now.
The Dilemma of Early Screening
I don’t know Amber’s background or medical history.
It’s just pretty rare for a 25-year-old female to be diagnosed with something that you usually find in someone who’s at least 60 years old, if not older.
And I think most people understand that.
So, the next question would be, “Okay, why not just screen for it? Obviously, it can happen.”
Ultimately, it looks like there’s a couple issues with this.
The Emotional, Financial, and Physical Costs
For one thing, because it’s so rare in that age group that testing everyone seems to be pretty draining, it puts a strain not just on financial resources, but it also causes unnecessary anxiety because if they see something pop up on imaging, now that person will start to wonder, could it develop into something worse?
Even though they could have probably just lived the rest of their life without even knowing about it. and they would have had a normal life.
The other component is that we would be exposing a lot of people to unnecessary radiation.
So really we have an emotional cost, an actual financial cost and potentially a physical cost.
So the medical system seems to be designed to give the most benefit to the most amount of people by noticing patterns and finding that signal in a sea of noise.
The interesting thing is that the research does show that the body often shows subtle signs, months or even years before the onset of diagnosis.
Hindsight and the “Needle in a Haystack” Reality
The thing about that is that it seems hindsight is 2020.
When they looked back on the imaging that was done in younger people were able to see some small changes in the pancreas about half the time.
The thing is, it wasn’t always obvious that it was a tumor or that it would lead to some sort of cancer. It was just something that they noted, some small change that occurred.
So again, this kind of goes back to potentially causing someone a significant amount of anxiety and potentially for no reason because that small change could have developed into a tumor, but most likely it wouldn’t have.
As we can see here, the chance of that finding becoming a pancreatic cancer is 0.05%.
So if you have a group of 2,000 young adults that actually did the imaging and found something in it, only one of them might actually get this type of cancer.
So, it’s a weird needle in a hay stack scenario where the needle might still be one of the hay sticks and the only real difference is that it might be a little bit bigger than the rest.
And since there doesn’t seem to be very strong research to tell us when to do more testing for young people, there is definitely a gray area here.
Identifying the “Meowing Box”: Recognizing Patterns in Your Symptoms
And this shows essentially the same thing that I just said where there could be small changes months or years before a tumor is obvious and at the same time those small changes might not develop into a tumor at all.
Maybe we can say it’s kind of like Schroinger’s cat where you don’t know if it’s dead or alive until you look inside the box.
But I would push that theory a little bit and I would say that you can know based on the clues.
So, for example, if you hear meowing coming out of the box or if you see the box move by itself, we can probably figure out that the cat is alive inside of the box.
We don’t actually have to open the box in order to figure that out.
We can use our other senses and other information. And when we collect enough information, we start to put it together and start seeing a pattern.
So, for example, if the box meowed once and then stopped, we would probably say that that was a bit weird for a box to meow.
And if we didn’t know that something like a cat exists in this world, we might open up the box to see what’s inside, or we might leave it alone.
But if we kept hearing meowing coming out of that box, then we’re going to know that there’s something inside to look for.
So, it’s really not just about one event. It’s how that event repeats itself and then how that event creates a pattern.
So, if you feel like you’re going in circles, the symptom appears, the doctor gives you some sort of medication, you get some sort of temporary relief, but it just keeps coming back. it doesn’t seem to be going away. You get this feeling that something else could be a miss.
You feel stuck in this loop. Then it’s probably time to dig a little deeper.
And most people intuitively know when something is not right.
From Passenger to Navigator: Building Your Advocacy Framework
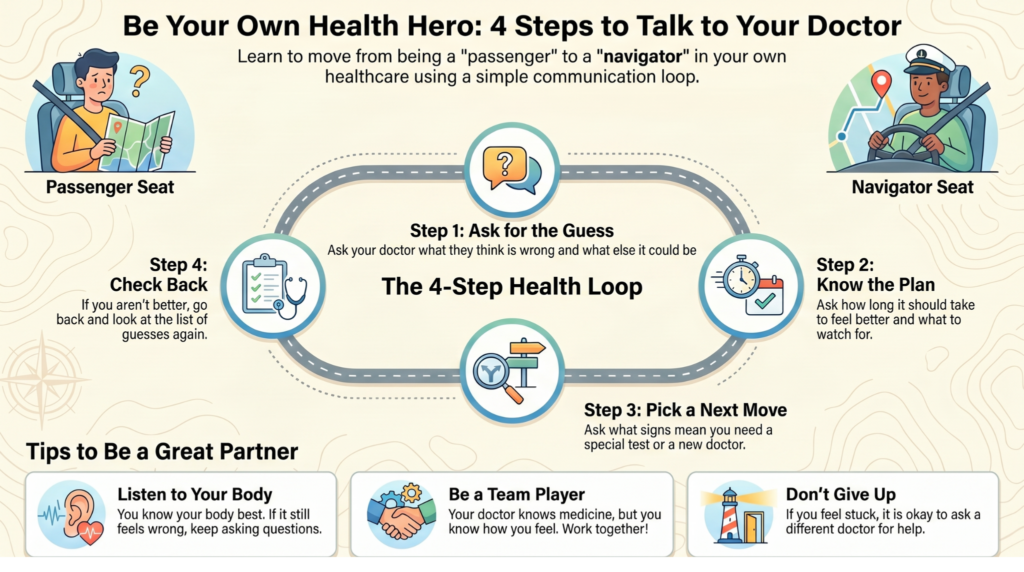
Moving from Noise to Signal
They just keep going back to the doctor until something is done.
And unfortunately, most of the time, I’ve seen people hope for some kind of breakthrough.
After all, the doctor should know what to look for, right?
They should know what to do. They should know where to send you. They should know what things to consider.
And again, all 100% correct.
However, you need to know the framework that your doctor is working with.
And that’s how self advocacy begins to develop because as soon as you appreciate the framework that thought process helps you see the map that your doctor is using and suddenly you become a navigator rather than just a passenger hoping to get to your destination.
That’s when we move from questions that stem from noise on the internet and we move towards questions that clarify a signal.
What else could this be? If this doesn’t improve, what’s our next step? What specific signs should I be looking out for? What would make you consider imaging like a CT scan or an MRI?
I feel questions like this help you develop a greater awareness. of yourself, the system and the collaboration you have between you and your doctor.
So this is the kind of loop that would be ideal because first of all you want to understand what is the current thinking.
The Four-Step Collaboration Loop
Step 1: Understand the Current Thinking
What is your doctor currently thinking at this moment? what is their leading diagnosis and what else could it be even if it is a rare disease?
Ask your doctor what is on that list of things that you’re considering. Are you including the rare stuff?
Step 2: Define Expectations
Next, you want to know what are the expectations.
If your doctor tells you a certain diagnosis, then you need to know what should improvement actually look like.
How long is that going to take?
Because you’re defining the parameters. You need to know if you need to take the next step. And if you do, you’ll be able to tell your doctor at your next visit, hey, I know we talked about this. I know you said improvement should look like this, and it’s been maybe two weeks. I haven’t seen any improvement.
Step 3: Identify Thresholds for Action
Now you’re escalating. What signs would prompt action? When should we recheck? When should we dig a little deeper? What would make you consider doing an ultrasound or a CT scan or an MRI? What would make you consider sending me to a specialist? What are the things I need to be looking for? What are the things that I need to tell them?
Step 4: Determine the Next Move
And I kind of put those together with step four because you’re basically asking that if the leading diagnosis doesn’t work based on the improvements that you said I should be experiencing by now, then what is the next step? How do we move forward? What’s our next move?
And this goes back to step one because now we need to step back and reassess.
Okay, maybe our leading diagnosis last time wasn’t correct. Maybe we need to do something else. Maybe we need to pursue something else on that list of possibilities. Or maybe the doctor has a really strong clinical judgment that the first diagnosis may still be correct. However, we might not have done enough to identify it and treat it properly.
So there could be those couple of pathways and every time you go home from the doctor you need to develop some of your own clarity.
Bridging the Gap: Combining Medical and Body Knowledge
Am I getting the answers that I need or is it just temporary relief? Is my baseline health actually improving? If nothing changes today, where does this path lead? Do I feel heard and understood by the doctor? And here you’re developing greater self-awareness? Is what I’m experiencing matching what they expected? Have I hit any of the thresholds we talked about? Am I following a plan or just hoping?
The point of all this is not to figure out if anything was missed from one visit. it’s that the pattern needs to trigger the next step.
And so your job becomes to identify the data that allows you to highlight that pattern to your doctor.
That pattern reveals your balance.
You could go to the doctor and they could just reassure you and tell you everything is fine without any additional testing.
However, if you’re experiencing the same symptoms over and over and it’s not going away and it seems to be getting worse, you got to keep asking the questions.
You got to keep going back because even though not every symptom is something serious, at the same time you want to do the proper leg work to make that it’s not something serious.
That’s not to say that your doctor hadn’t already considered the serious components of the issue.
However, this is all about being on the same page with the doctor just as much as it is about the doctor being on the same page with you.
This is a collaboration.
It has to be a collaboration because your doctor has the medical knowledge and you have your body knowledge.
If your body continues to send you signals that basically say, “Hey, something is still going on here.” And frankly, I don’t think it’s getting any better. And you need to collect that information and bridge that gap to let your doctor know about it.
The Path Forward: Staying Persistent and Hopeful
Because most serious conditions don’t start as emergencies.
They start as something small and it doesn’t quite go away and it just keeps nagging at you the whole time.
So the goal is not to panic.
The goal is to stay curious.
The goal is to gain clarity.
The goal is to remain persistent.
The goal is to listen to your body and work with your doctor to figure out what’s actually going on.
The goal is to let your body guide you.
I know it’s hard sometimes.
Actually, it’s hard a lot of the times.
Many people go to the doctor trying to get answers and walk away utterly frustrated, feeling unheard, disappointed, dismissed, kind of shrugged off like, “Oh, you don’t know what you’re talking about.”
And it can be very easy to just accept that.
But Amber’s message is an important one. You have to keep pushing.
If you know something’s wrong, you have to keep pushing.
Unfortunately, it is kind of a numbers game.
You might have to look for a second or third or 10th opinion.
That might be overkill.
However, if you’re working with your doctor in a collaborative way where you’re asking the questions that help you see things more clearly, then you are staying true to Amber’s positivity.
You are staying true to her message.
And I think at the base of it all is hopefulness.
So, I think I’m going to end this by saying stay hopeful.
Thank you for reading. I hope this helped.
Please leave me some comments if you want to carry on the conversation.
Health and Wellness coaching
Would it be a bad idea to work together now?
If You’re Not Ready Yet, That’s OK.







